Lunch & Learn: Neurobiology & GBV/IPV

Halifax: The future of social work regulation in NS
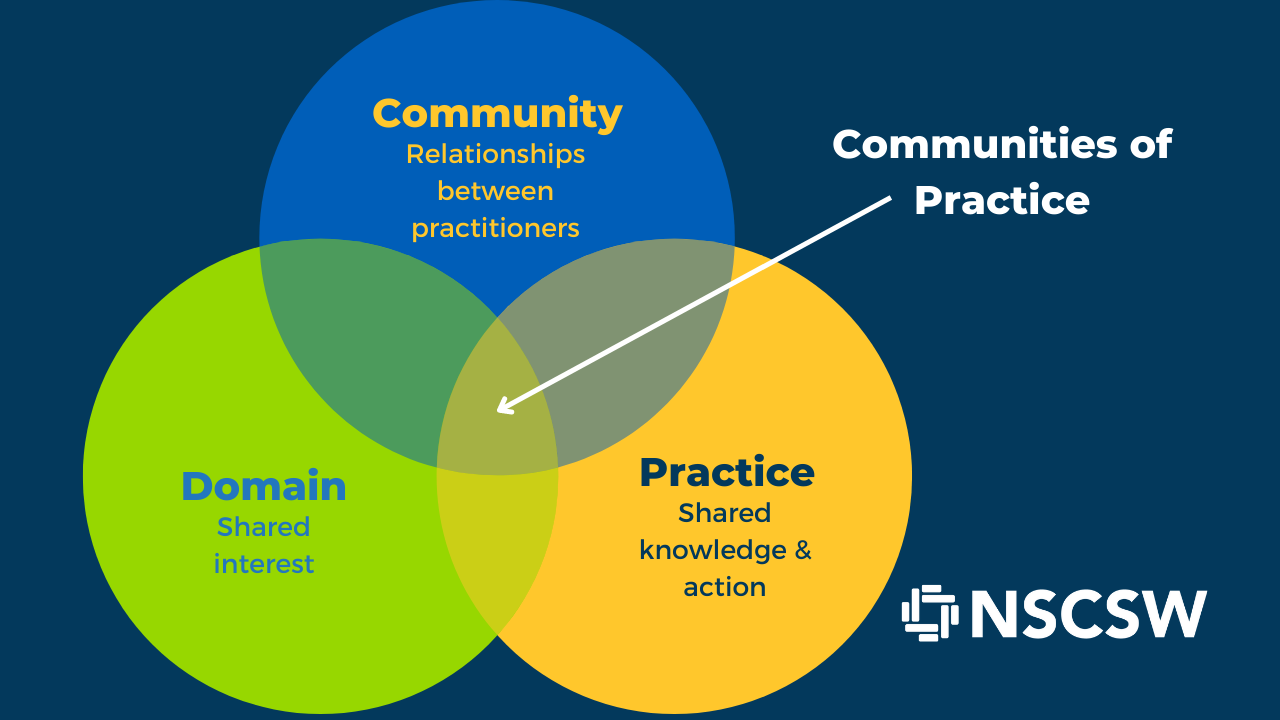
Connections: Communities of Practice
Lunch & learn: Exploring anti-fat bias in child & family wellbeing

Yarmouth: The future of social work regulation in NS

Bridgewater: The future of social work regulation in NS

Navigating the PHIA amendment

As social workers, we often face complex decisions when we must balance client privacy with the need to prevent harm. To help us navigate these high-risk situations, an important change has been made to the Nova Scotia Personal Health Information Act (PHIA). Effective April 1, 2026, the word “imminent” was removed from the provision that allows the discretionary disclosure of personal health information (PHI) without consent.
We want to ensure you understand exactly what this amendment means for your daily practice, and how our professional ethics and clinical standards guide these difficult choices.
What is Changing Under PHIA?
Previously, Section 38(1)(d) of PHIA allowed you to disclose PHI without a client’s consent if you have reasonable grounds to believe it will avert or minimize an “imminent and significant danger” to health or safety.
After April 1, 2026, the requirement for the danger to be “imminent” disappeared. The updated section allows disclosure if you believe, on reasonable grounds, that sharing the information will avert or minimize a significant danger to anyone.
This change was introduced as part of the Protecting Nova Scotians Act (Bill 127). Advocacy groups highlighted that waiting for a danger to become “imminent” created unnecessary barriers. By removing this word, the law empowers you to share vital, limited information sooner to prevent a crisis from escalating. This update also aligns Nova Scotia with provinces like Alberta and Manitoba, which have removed similar requirements to support better safety interventions.
What This Means for Your Practice
This amendment lowers the legal threshold for sharing information, but it does not change the core responsibilities of your role. Here is what you need to consider:
- A Shift in Urgency: Urgency still matters, but you no longer need to wait until a danger is on the verge of occurring before you act.
- Reasonable Grounds: You must base your decision on professional judgment, client history, collateral information, and thorough assessments.
- Discretionary Action: Disclosure remains a discretionary choice, not a mandatory requirement. You must assess each situation individually.
- Minimum Necessary: You should only share the minimum amount of information required to address the danger.
Let Our Code of Ethics Guide You
The NSCSW Code of Ethics and Standards of Practice & Clinical Standards of Practice provide a strong framework for making these discretionary disclosure decisions. When applying the new PHIA guidelines, lean on these foundational principles:
Balancing Privacy and Protection
Maintaining Privacy and Confidentiality (Value 6) stresses our professional obligation to safeguard client information. Standards 6.1 and 6.4 require us to disclose confidential information only with valid consent or when legally justified. The PHIA amendment provides that legal justification, but we must remain transparent about the limits of confidentiality and share only what is absolutely necessary.
Respecting Dignity While Upholding Safety
Respecting the Dignity and Worth of All People (Value 1) emphasizes client autonomy and self-determination. However, Standard 1.9 requires us to uphold the right of every person to be free from violence. Navigating the tension between respecting a client’s choices and protecting them or others from harm is a central ethical dilemma. The removal of “imminent” allows you to act proactively to uphold safety while minimizing harm.
Preserving Integrity and Valuing Relationships
Valuing Human Relationships (Value 4) asks us to weigh the risk of damaging the therapeutic alliance against the risk of danger. Preserving Integrity in Professional Practice (Value 5) ensures we act with honesty, responsibility, and accountability. You must trust your clinical expertise and situational awareness to make these tough calls.
Promoting Social Justice and Competence
Promoting Social Justice (Value 2) calls on us to advocate for the safety and well-being of our communities. Furthermore, Providing Competent Professional Services (Value 7) and Standard 7.2 remind us to seek appropriate guidance when a situation feels beyond our immediate scope.
Key Next Steps for Social Workers
As you adjust to this change, keep a few practical considerations in mind:
- Check Mandatory Duties: Always ask yourself if a separate mandatory duty to report exists, such as under the Children and Family Services Act or the Adult Protection Act.
- Identify the Best Intervener: Determine who is best positioned to act. This might be law enforcement, a parent, or someone within the client’s immediate circle of support.
- Document Everything: You must meticulously document any disclosure made without consent in the client’s health record. Clear documentation demonstrates your professional judgment and ethical decision-making process.
While the concept of urgency still plays a vital role, the updated PHIA gives you more room to intervene before harm occurs. We encourage you to consult your manager, director, or legal and privacy services whenever you face a challenging disclosure decision.
Workshop: Anger Management (Halifax)

Pjila’si: Community of practice for Mi’kmaw & Indigenous social workers

63rd Annual General Meeting

Sign up for Connection
CONNECTION is the official newsletter of the Nova Scotia College of Social Workers.